Key points:
- Gene therapy for primary immunodeficiency (PI) modifies hematopoietic stem cells from the bone marrow to restore a working immune system.
- Currently, gene therapies for Wiskott-Aldrich syndrome (WAS) and leukocyte adhesion deficiency type I (LAD1) are the only FDA-approved gene therapies available in the U.S. for PI. Other gene therapies are available through clinical trials only.
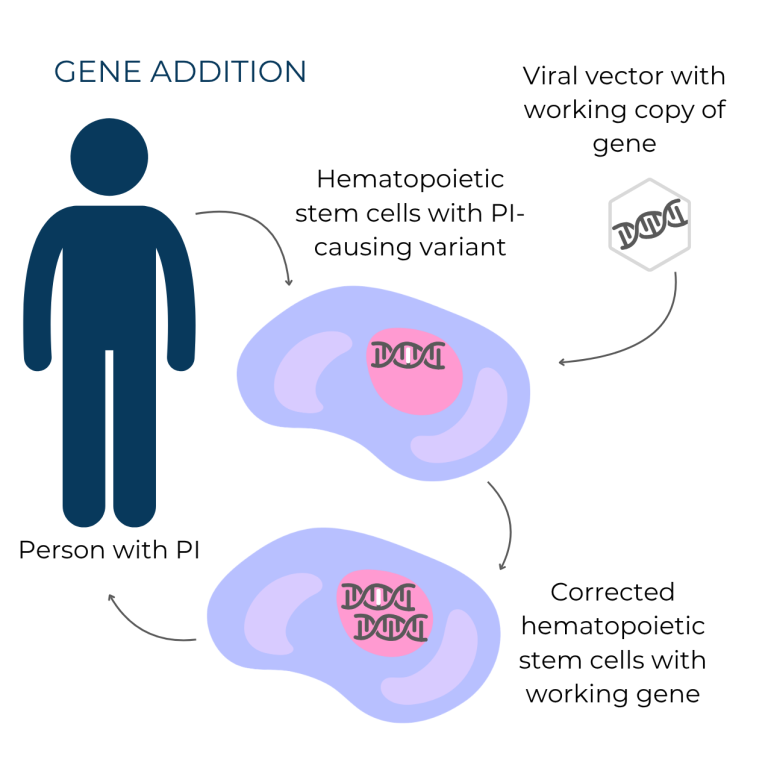
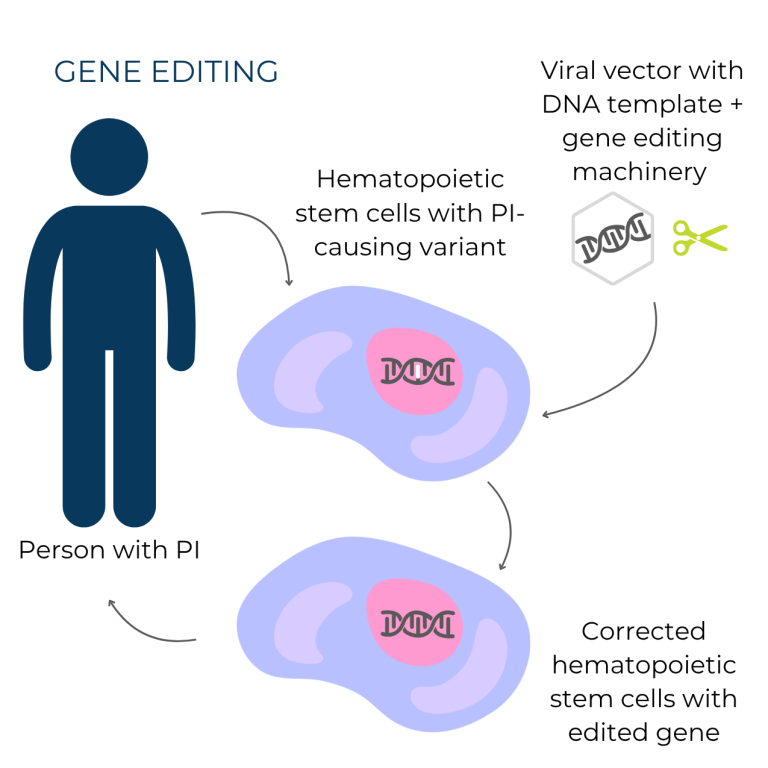
- There are two main strategies for PI gene therapy: gene addition, which inserts a working gene copy into cells, and gene editing, which directly corrects PI-causing genetic variants. Both methods use viral vectors to deliver the therapy to cells.
- Gene therapy has the potential to treat many types of PI and it is likely that gene therapy will be the standard treatment for severe PI in the future.
History of gene therapy to treat PI
Gene therapy has been used in clinical trials to treat people with several types of severe combined immunodeficiency (SCID), hereditary angioedema (HAE) type 1, X-linked chronic granulomatous disease (X-linked CGD), and leukocyte adhesion deficiency-1 (LAD-1). In 2025, Waskyra for WAS became the first gene therapy for PI approved in the U.S.
Gene therapy for ADA-SCID
The first clinical trial for gene therapy was at the National Institutes of Health in 1990 and treated a 4-year-old girl with ADA-SCID [6]. The design of this first trial focused on adding the ADA gene sequence to her T cells with a viral vector. She received multiple infusions of her own gene-modified T cells over a two-year period. Her T cell counts and function rapidly rose to normal levels after treatment. Although her total number of T cells eventually fell below the range for healthy individuals after about 9 years, she remained healthy and free from serious infections. The working ADA gene remained in 20-40% of the patient’s T cells at last report, twelve years after gene therapy [7].
After this initial clinical trial showed that gene therapy could be done safely and that gene-corrected T cells could survive and function for years, additional clinical trials began to treat other children with ADA-SCID by targeting the long-lasting hematopoietic stem cells from the bone marrow. In terms of providing a working immune system, the results have been excellent. Most of the nearly 100 individuals treated for ADA-SCID reached a significant, long-lasting increase in T and B cell counts and have had a remarkable improvement in immune function [8], [9].
In 2016, the European Medicines Agency (EMA) approved Strimvelis, a gene therapy for ADA-SCID that uses a retroviral vector. Thirty-three patients were treated with Strimvelis before reports in the fall of 2020 that one patient developed leukemia, a type of blood cancer, four years after treatment due to insertional mutagenesis [10]. Insertional mutagenesis is when DNA from the viral vector activates other genes near where the new, working gene has been added to the stem cell’s chromosome. Depending on which genes are nearby, activating these genes can make a stem cell more likely to become cancerous. Gene therapy research now uses other vectors that are less likely to cause insertional mutagenesis.
EMA issued a direct healthcare professional communication in early 2021 advising clinicians to follow patients closely for signs of leukemia [11]. Strimvelis remains authorized in the European Union.
Gene therapy for other PIs
The first gene therapy trials for X-linked SCID, X-linked CGD, and WAS also used retroviral vectors to add working versions of the affected genes into hematopoietic stem cells. While these trials resulted in restored immune function for the majority of treated individuals, a substantial number of people went on to develop leukemia in the years following treatment due to insertional mutagenesis caused by the viral vector.
Recent trials for several types of PI use updated viral vectors, called lentiviral vectors, that are designed to avoid insertional mutagenesis. These therapies resulted in immune benefits that are similar to, or even better than, those seen in earlier trials. To date, no cases of leukemia have been associated with lentiviral vector-based gene therapies for PI. However, there have been cases of insertional mutagenesis in a lentiviral vector trial for a metabolic disease called adrenoleukodystrophy [12]. This complication underscores the importance of ongoing monitoring and further advancements in the technology to ensure safety.
Waskyra for WAS and Kresladi for LAD1 use lentiviral vectors and both carry a warning that healthcare providers should monitor all treated individuals for cancer for at least 15 years after treatment [13].
Limitations of gene therapy
Gene therapy shares some limitations with HSCT. Like HSCT, gene therapy will fix problems specific to the cells made from the modified hematopoietic stem cells, but problems outside of the blood or immune system may not be corrected. As a result, PIs that affect cells outside the blood may not be fully treated. In addition, sperm and egg cells are also not modified, so a person who has had successful gene therapy can still pass PI-causing variants on to their children. Gene therapy also cannot reverse or repair damage already caused by PI, such as lung damage from severe infections.
Unlike HSCT, which is a general therapy that can treat a wide variety of PIs, gene therapy is more specialized and requires a tailored approach for each specific type of PI. This specialization makes gene therapies some of the most expensive treatments available. Health insurance companies may not cover them, even after FDA approval. Furthermore, gene therapy is limited to treating PIs caused by variants in a single, identified gene.
Despite these challenges, growing experience with gene therapy demonstrates its potential to successfully treat PI through gene addition or editing. As the field continues to develop, gene therapy may become a treatment option for many severe types of PI in the future.
Gene therapy products approved in the U.S.
Kresladi
Marnetegragene autotemcel.
Approved to treat: Leukocyte adhesion deficiency type 1 in people without a matched, sibling donor suitable for hematopoietic stem cell transplant (HSCT).
Ages: N/A.
Waskyra
Etuvetidigene autotemcel.
Approved to treat: Wiskott-Aldrich syndrome (WAS) in people without a matched, related donor suitable for hematopoietic stem cell transplant (HSCT).
Ages: 6+ months.
Latest gene therapy resources
This page contains general medical and/or legal information that cannot be applied safely to any individual case. Medical and/or legal knowledge and practice can change rapidly. Therefore, this page should not be used as a substitute for professional medical and/or legal advice. Additionally, links to other resources and websites are shared for informational purposes only and should not be considered an endorsement by the Immune Deficiency Foundation.
Adapted from the IDF Patient & Family Handbook for Primary Immunodeficiency Diseases, Sixth Edition.
Copyright ©2019 by Immune Deficiency Foundation, USA
Sign up for updates from IDF
Receive news and helpful resources to your cell phone or inbox. You can change or cancel your subscription at any time.